Breast Augmentation Surgeries in Gold Coast & Toowoomba
Breast augmentation most frequently involves the insertion of a breast implant. Associate Prof Magnusson increases using breast fat grafting for breast enlargement and shaping in combination with breast implants or on its own to enhance the breasts.
Breast implants: Silicone or Saline
Associate Prof Magnusson uses silicone gel implants. Breast implants differ in a number of ways. The Most obvious difference is the substance inside the implant, either Silicone or Saline. Silicone breast implants tend to feel more natural, have fewer aesthetic concerns such as rippling and tend to last longer than saline implants (silicone outer layer filled with saltwater). The silicone implants he uses have cohesive gel like Turkish Delight because of how the gel sticks together. Older generation silicone implants had a liquid silicone gel with a consistency more like honey. Cohesive gel implants tend to still stay together even with implant rupture, and there is a reduction in problems such as silicone bleed and silicone migration after extracapsular spread. The next most obvious difference is the surface of the implant shell. There are smooth and textured breast implants. Textured breast implants have been used historically used in many regions due to a lower rate of capsular contracture (hardening), and implant migration (movement out of position). These are the commonest reasons for implant reoperation until rupture becomes more common as we approach and move past 10 years. More recently in 2017, research that A/Prof Magnusson has helped spearhead has revealed the true association between textured breast implants and Breast Implant-Assocaited Anaplastic Large Cell Lymphoma. In Australia there is no known case of BIA-ALCL associated with smooth breast implants in isolation. All Australian BIA-ALCL patients have had exposure to textured breast implants.
Different implant types have different risk profiles and performance benefits. At your consultation implant selection is based on a discussion to balance these risks and benefits in reference to your individual requirements.
Breast Augmentation Implant Shape
Implants are either round or anatomical or teardrop shaped. Importantly all shaped implants are textured and therefore carry the rare risk of BIA-ALCL. For the majority of women, implant shape is not vital and different implants can be selected according to goals on the basis of other characteristics of the implant such as gel firmness and implant fill. High and extra high projection implants will always have the most significant difference in the shape of the upper pole when comparing round and shaped implants.
In some instances, a shaped implant may be considered such as:
- Slim patient with a very small amount of breast issue desiring a natural outcome
- High or extra-high projection implants with a large but natural shape
- Significant breast asymmetry or developmental deformity
- Women with a low nipple position may consider a shaped implant to give better support of the nipple to avoid additional mastopexy surgery
- Desiring a natural outcome
- Breast reconstruction following mastectomy
Implant surface
Implants have either smooth or textured surfaces. Textured breast implants have been used historically used in many regions due to a lower rate of capsular contracture (hardening), and implant migration (movement out of position). These are the commonest reasons for implant reoperation until rupture becomes more common as we approach and move past 10 years following implant insertion. More recently in 2017, research that A/Prof Magnusson helped spearhead revealed the true association between textured breast implants and Breast Implant-Associated Anaplastic Large Cell Lymphoma. In Australia there is no known case of BIA-ALCL associated with smooth breast implants in isolation. All Australian BIA-ALCL patients have had exposure to textured breast implants. Different implant types have different risk profiles and performance benefits. At your consultation implant selection is based on a discussion to balance these risks and benefits in reference to your individual requirements.
All anatomical implants are textured to reduce the likelihood of implant rotation. Round implants can be either smooth or textured. In some circumstances, implant migration has a higher risk and textured implants will be considered and used more frequently although the use of tissue scaffolds with breast implants can be used to stabilise implant position if migration occurs and especially if it is recurrent. A/Prof Magnusson selects implants in an individual basis taking into account goals, the breast that is already present and a full discussion of risk and benefits of different options. Because of the rare risk of BIA-ALCL he now mainly uses smooth implants.
Breast Implants v. Fat Grafting:

Breast implants allow us to achieve a substantial volume increase that can’t be achieved with fat grafting in a single episode. Autologous Fat Grafting can be very useful but when we compare outcomes between implants and fat we can consider the analogy of breast sand castles with either wet or dry sand. Wet sand comes out of the bucket with a defined shape and projection, this is the implant. Dry sand spreads, fills hollows well but doesn’t give the same structure to the breast, this is fat grafting. Fat is however excellent for defined goals such as narrowing a cleavage in association with breast implants, mild breast asymmetry, low volume filling of the upper pole of the breast and improving contour irregularities especially in reconstruction of developmental disorders and after breast cancer. While there are risks with breast fat grafting, once it is in and stable it generally needs no ongoing surgery. The best outcomes with fat grafting may require more than one operation for ideal outcomes. Breast implants require monitoring and will eventually need to be replaced. Increasing breast size with fat grafting involves removing fat from other areas such as the tummy, love handles, waist and thighs by liposuction. This fat is then processed and returned to the breast.
Autologous fat grafting has several limiting factors. We can only harvest fat if there is enough to remove without causing a new problem from liposuction. We can only put back about as much fat as the volume of the breast itself. Although the size change will be substantial initially with all of the fat and also with bruising and swelling, about a third goes over 2 months with the resolution of swelling and another third goes over 6 to 9 months as half of the fat disappears through a process of fat necrosis. While fat grafting makes definite measurable changes, it may feel as though it has “all gone” due to the gradual reduction over the first 6 months. The fat that remains however is permanent.
Breast implant considerations
- Significant volume enhancement required
- Breast implants are not life devices and will eventually require revision

Breast fat grafting will only allow us to achieve a mild to moderate increase in size but is especially useful to improve the shape and as part of a surgical plan for breast reconstruction for congenital breast deformities such as tuberous or constricted breasts and following breast cancer. Fat grafting can be used to achieve particular goals such as narrowing the cleavage and filling the upper part of the breast in particular when a shape improvement rather than significant volume change is desired. Fat grafting can be repeated at a later stage to obtain further volume change.
Breast fat grafting considerations
- Abnormalities of breast shape such as tuberous or constricted breast
- As part of breast reconstruction following breast cancer treatment
- The goal is for shape change rather than substantial volume increase: regain upper pole fullness following pregnancy or to narrow the cleavage
- Fat grafting is frequently used by Associate Prof Magnusson as a component of explant surgery
Breast Implants v. Fat Grafting:
Undertaking cosmetic surgery (also known as aesthetic plastic surgery) is an intensely personal and private decision that can very positive effects. Success comes from helping individual patients clarify their goals and then creating a bespoke plan to achieve them. With a combination of communication, experience and knowledge, A/Prof Mark Magnusson has helped many patients across Brisbane, Toowoomba and Gold Coast. Let Dr Magnusson help you with your aesthetic journey.
Your breast augmentation consultation
The outcome of breast enlargement surgery can be something that patients find exciting and rewarding however it is always important to understand that this is real surgery with real risks and an anticipated recovery period. The outcome of surgery will depend upon the individual plan being created, a technically well-performed procedure and a patient following the post-operative instructions to minimise the risk of problems.
To develop the best operative plan for you we will need to determine the optimal breast size according to what you already have and what you wish to achieve. We will need to determine the best incision and the best pocket for the implant as well as evaluating whether additional procedures such as a mastopexy or autologous fat grafting may be considered to maximise the outcome and what will differ if we don’t employ these additional tools.
In addition to these elements relating to your breast, we will need to explore your medical history including prior breast surgery or problems with other operations.
Photographs are routinely taken prior to your consultation and form an integral part of your confidential medical record. Photographs make a very useful tool during the consultation to compare outcomes from other patients with achievable results for you. Photographs are not seen by others outside the clinical team under any circumstances without your express consent.
How much does breast augmentation cost?
It isn’t always possible to obtain an accurate cost for breast augmentation surgery without scheduling a consultation with a qualified plastic surgeon such as A/Prof Magnusson. There are several factors that contribute to the overall cost. While the surgical cost from A/Prof Magnusson is consistent, other charges vary including the anaesthetist, hospital and breast implants. Many patients choose to combine augmentation with other procedures such as a breast lift or fat grafting, which can also impact the final cost of the surgery. Since breast augmentation is usually purely cosmetic, patients will not be able to apply for a Medicare rebate. However, if augmentation is required following a mastectomy, tuberous breast deformity or significant breast asymmetry (difference in size between the breasts), both private health insurers and Medicare may cover a some of the costs for both surgery, implants and also adjunctive procedures such as mastopexy and fat grafting. A/Prof Magnusson can hep determine if there will be a rebate from Medicare/Health Fund for your surgery – the rest of the costs will be out of pocket.
Breast Augmentation Patient Information
Risks
Are you considering a Breast Augmentation? All surgery carries risking breast augmentation is no different. Associate Professor Magnusson discusses the risks of breast augmentation procedures in the video link below. Half of reoperations after breast implants are due to changes in the breast without problems due to the implant. These are due to changes associated with normal life events such as weight fluctuations, pregnancy and ageing. The three commonest reasons for reoperation due to implants are capsular contracture (hardening), migration (movement our of position) and eventually rupture which is uncommon prior to 10 years but increasingly common after. About 1 in 10 have had reoperation by 10 years and half still have their implants at 15 years. In addition all procedures carry general risks of surgery such as bleeding and infection.

Considerations
Associate Professor Magnusson discusses the considerations required for a Breast Augmentation procedure, including the implant type, size and shape, the aesthetic goals of the results, and if any other procedures should be combined with your Breast Augmentation.

Limitations
Associate Professor Magnusson discusses the importance of having realistic expectations with a Breast Augmentation procedure, and the limitations involved depending on your procedural choice, breast size, shape and the breast skin & tissue.

Restrictions
When choosing if a surgery is right for you, it’s important to note the post-operative restrictions that will be required to ensure the best recovery possible. Associate Professor Magnusson covers the different type of restrictions that will be required for post Breast Augmentation surgery, and how that may affect you.

Size
If you are considering a Breast Augmentation, you may be wondering what your bra and cup size might be post operation. Associate Professor Magnusson gives a rough estimate of what can be expected after a Breast Augmentation.

Changes
Dr Magnusson discusses common questions asked regarding changes in the breast and nipple function after surgery, such as sensation in the nipple as well as breast feeding functionality. These are dependant on numerous factors which Associate Professor Magnusson covers.

Complications
With any surgery, it’s important to understand both the short term and long term risk of complications and to be aware of any revisions that might be required in the instance of a complication. Associate Professor Magnusson discusses the different complications that may be a result of a Breast Augmentation surgery and what may be required to correct these complications.

Surgery & Smoking
When considering a Breast Augmentation surgery, smoking may affect your healing process of the wound most especially if mastopexy is included in your surgical plan. Associate Professor Magnusson discusses the risks associated with smoking within the weeks leading up to surgery, as well as the recommended time period to avoid smoking before and after surgery.

Implants vs Fat Grafting
When considering a Breast Augmentation, one may compare the procedure with others, such as Fat Grafting of the breast. Associate Professor Magnusson discusses the similarities and differences between the two surgeries, and what may be best for you depending on factors such as your breast shape and size, where your breasts sit, and your desired results.

What you need to know about BIA-ALCL
Breast Implant-Associated Anaplastic Large Cell Lymphoma (BIA-ALCL) is one of the risks associated with breast implants, with some implants resulting in higher risks than others. Associate Professor Magnusson discusses what BIA-ALCL is and which implants may result in higher risks of BIA-ALCL, and what preventative measures may be made to reduce the risks.

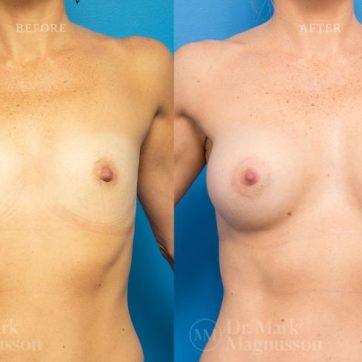
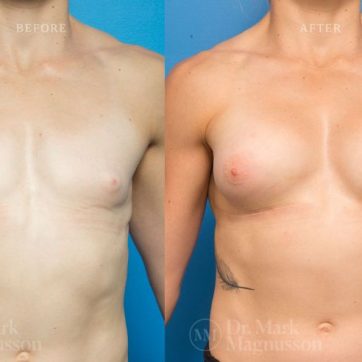
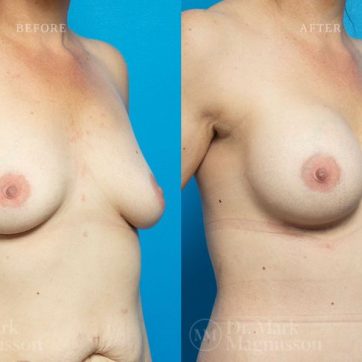
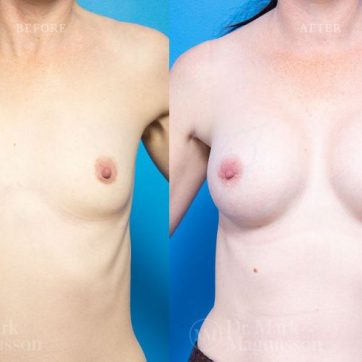
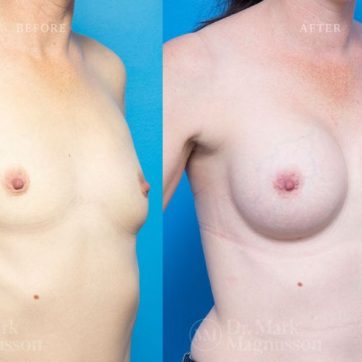
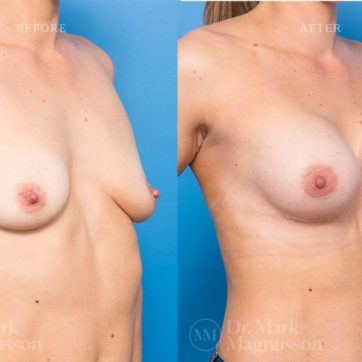
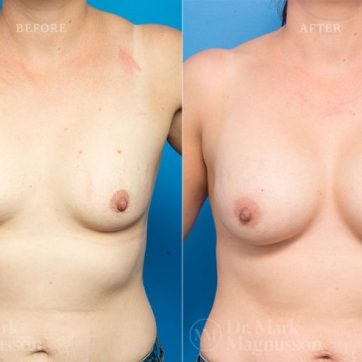
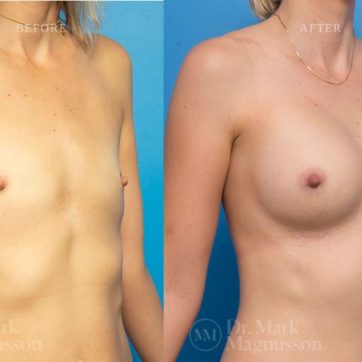
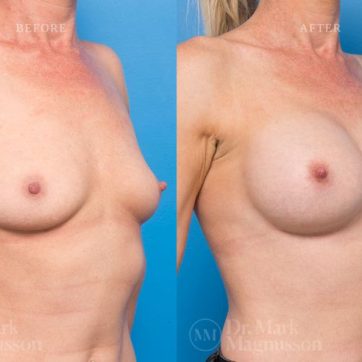
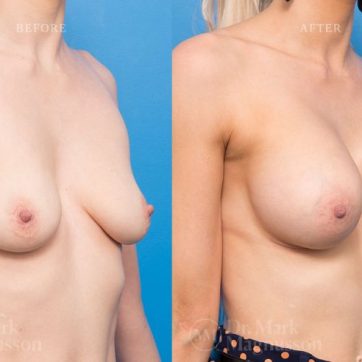
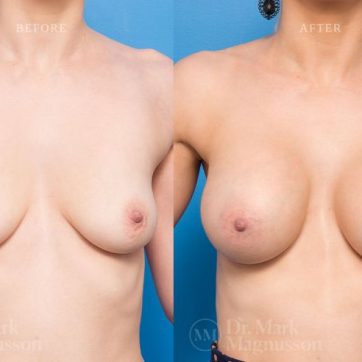
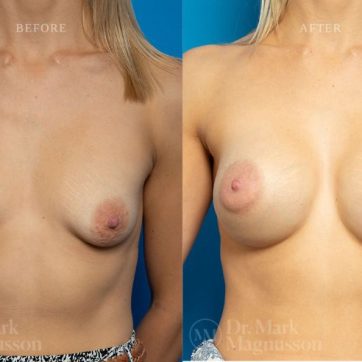
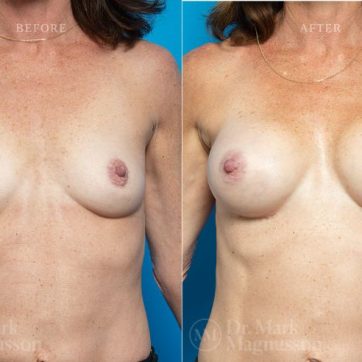
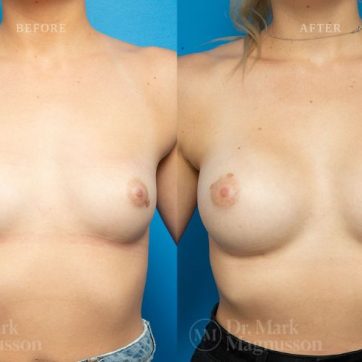
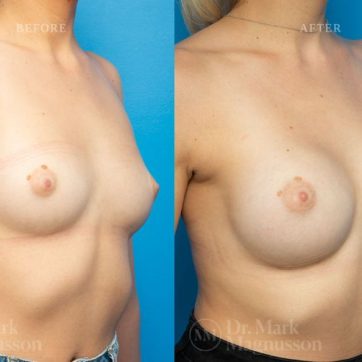
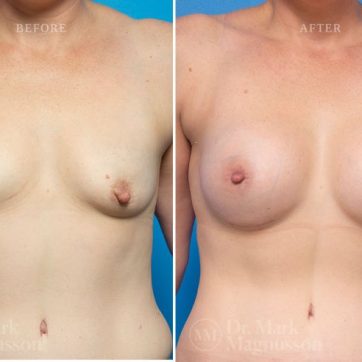
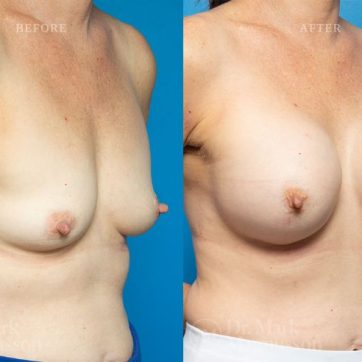
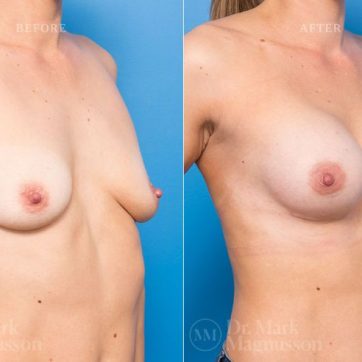
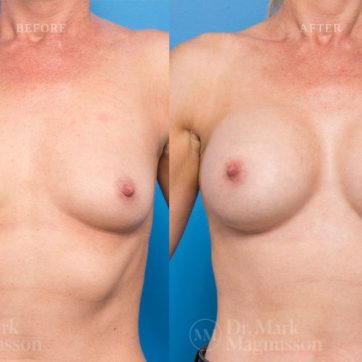
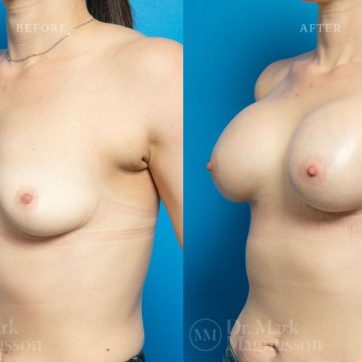
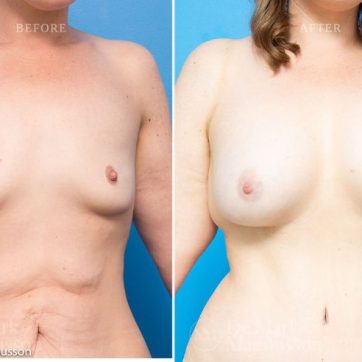
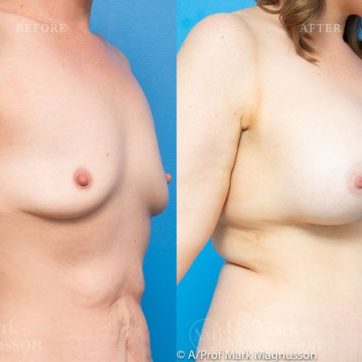
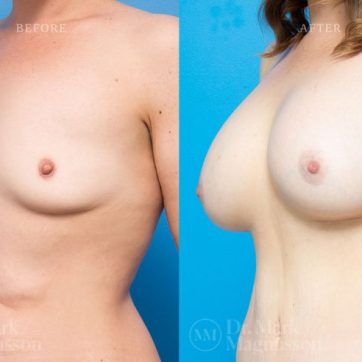
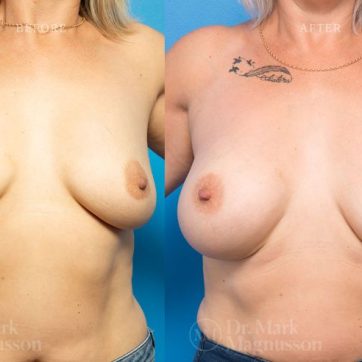
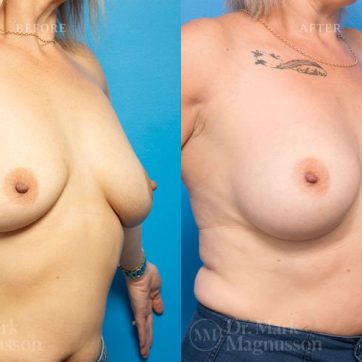
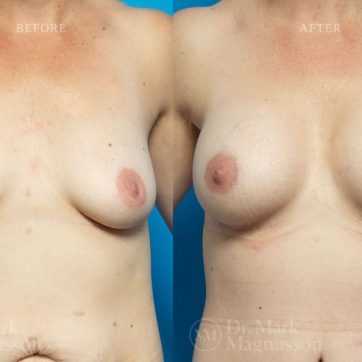
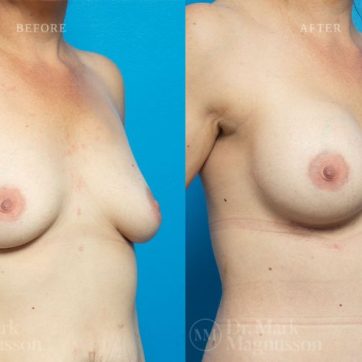
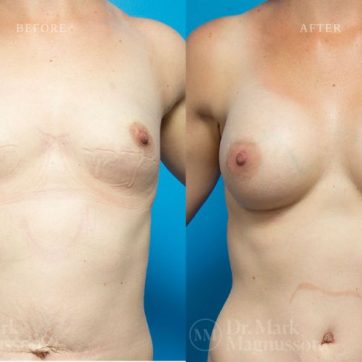
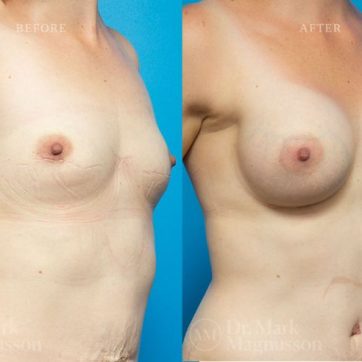
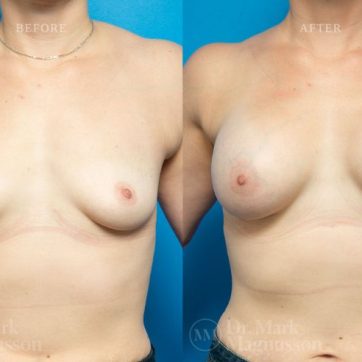
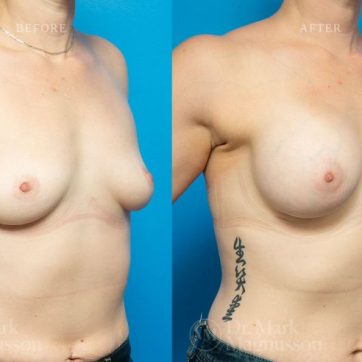
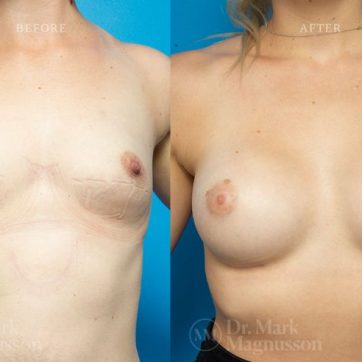
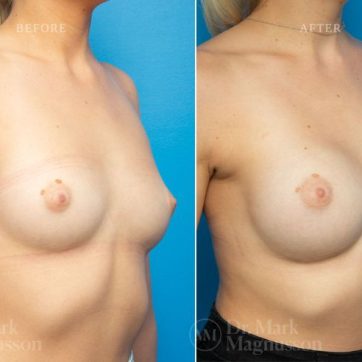
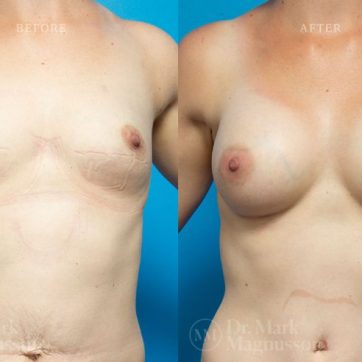
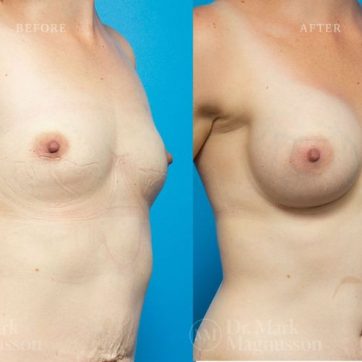
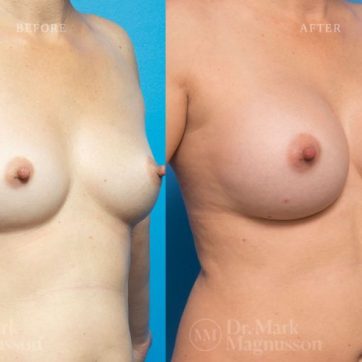
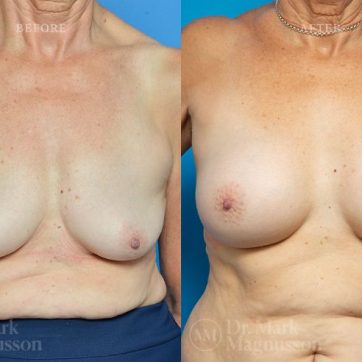
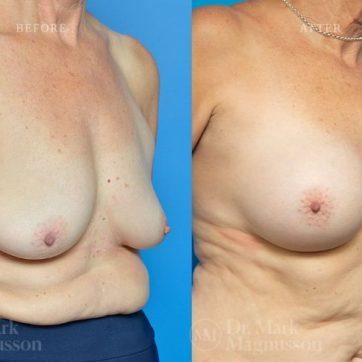
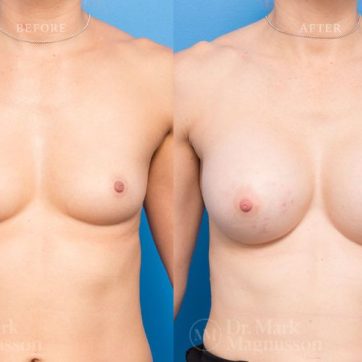
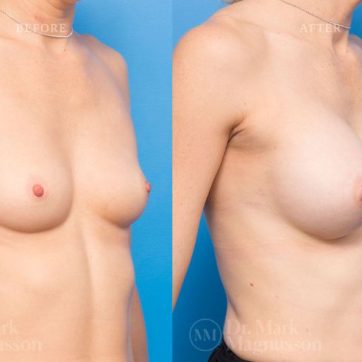
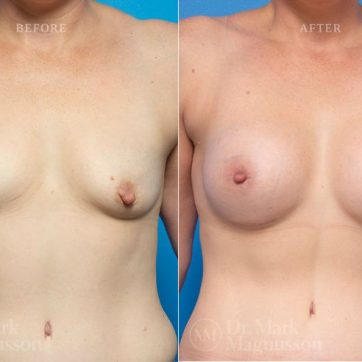
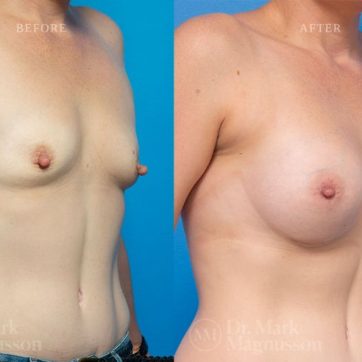
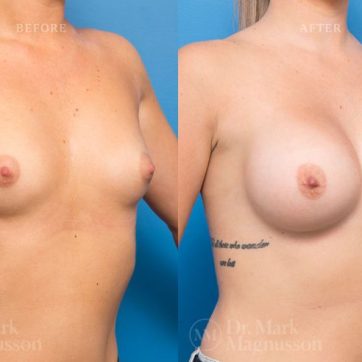
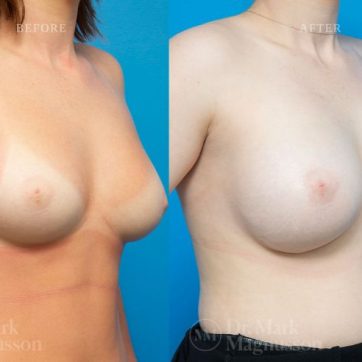
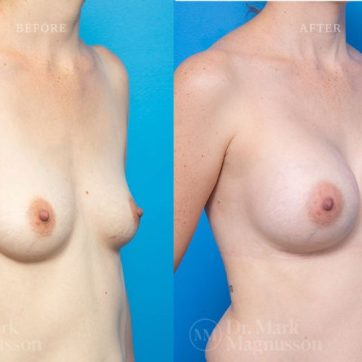
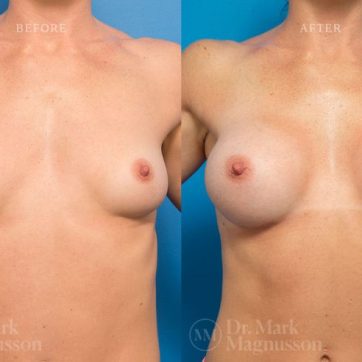
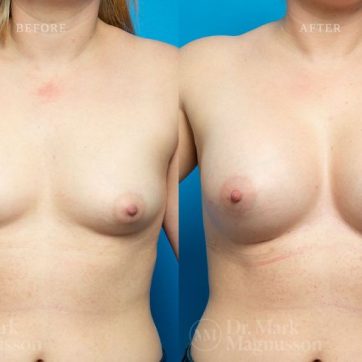
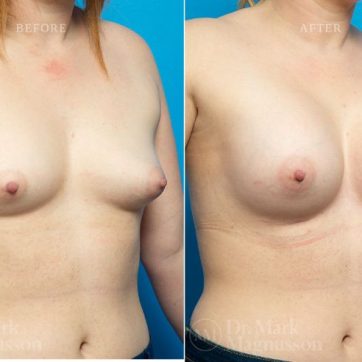
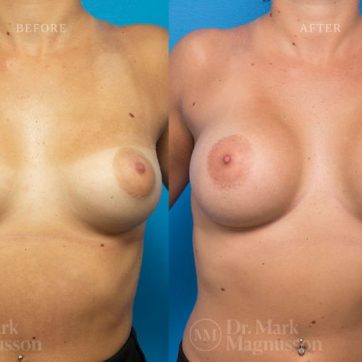
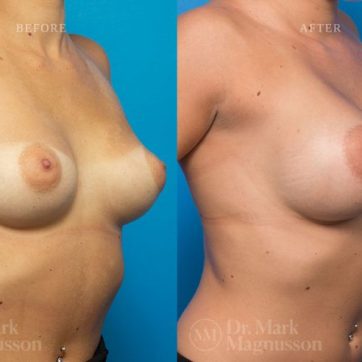
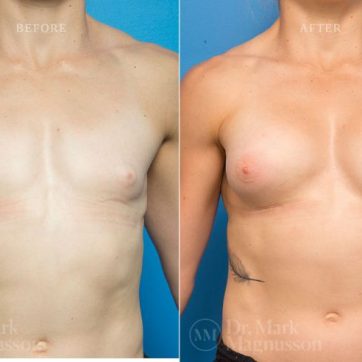
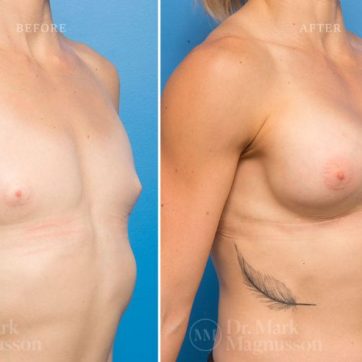
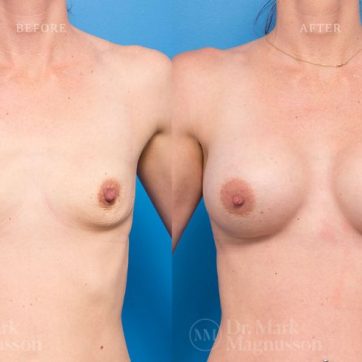
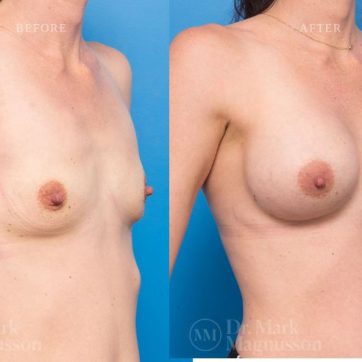
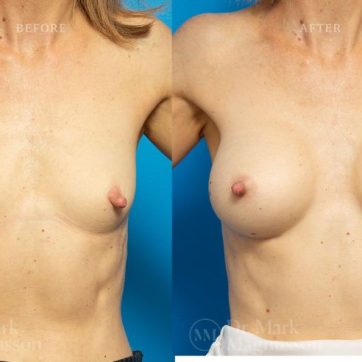
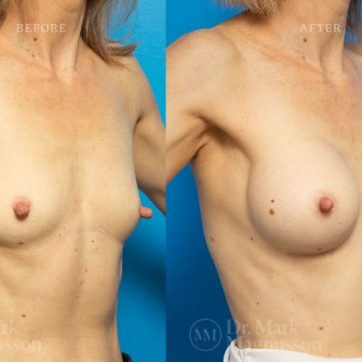
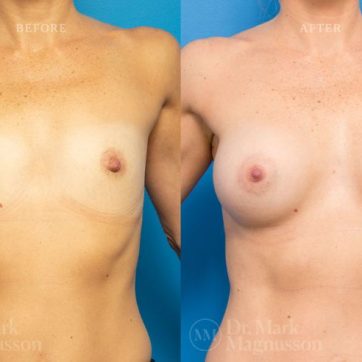
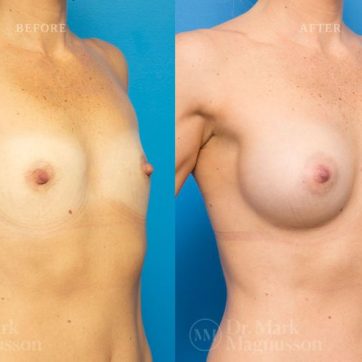
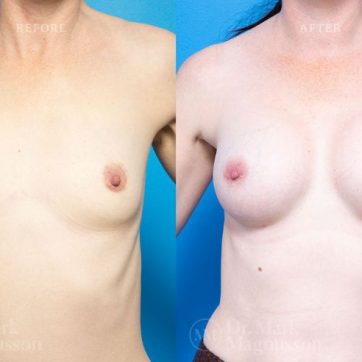
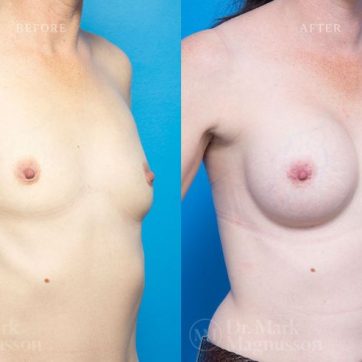
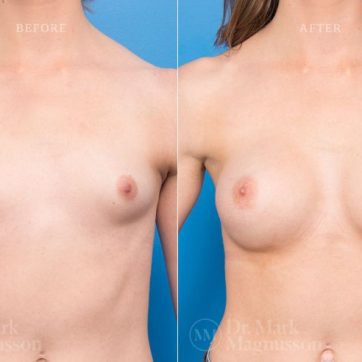
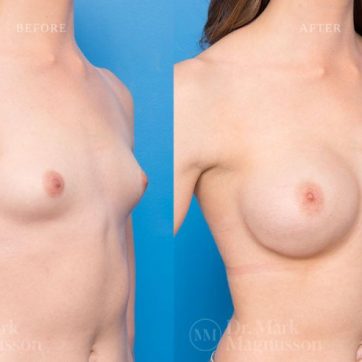
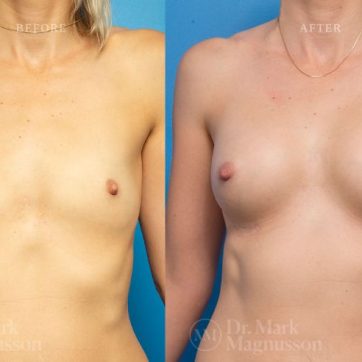
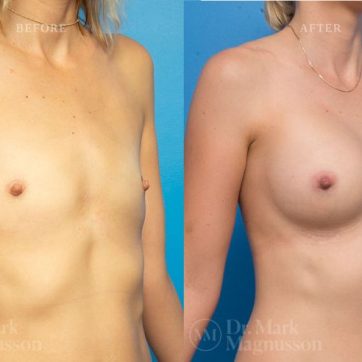
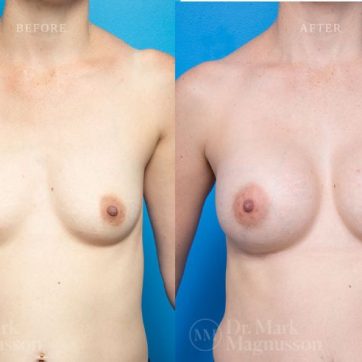
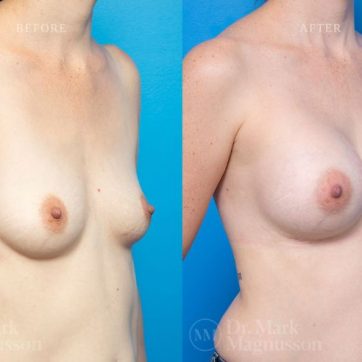
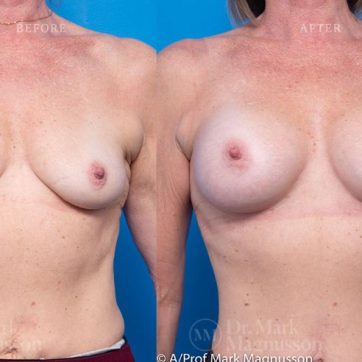
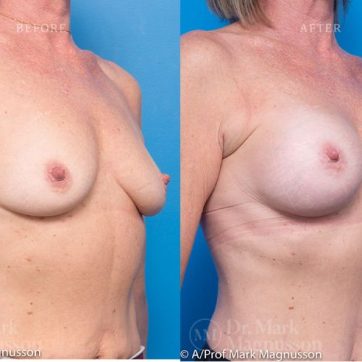
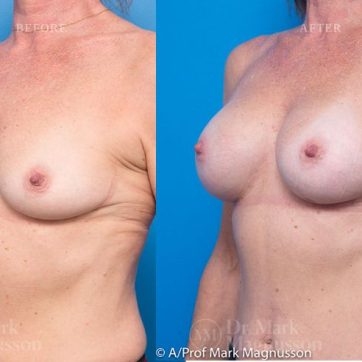
Breast Augmentation Before and After Gallery
The outcomes shown are only relevant for this patient and do not necessarily reflect the results other patients may experience, as results may vary due to many factors including the individual’s genetics, diet and exercise.
Book an appointment for breast augmentation in Brisbane, Toowoomba or the Gold Coast
A/Prof Magnusson can discuss the breast enhancement procedure with you and provide you with information regarding risks and recovery times at your initial consultation. He has assisted patients in Brisbane and throughout Queensland. Request an appointment by contacting reception at either his Toowoomba or Gold Coast clinics today.
Breast Augmentation – Frequently Asked Questions
How is breast augmentation surgery planned?
Planning breast augmentation surgery requires a structured, individualised consultation process. A/Prof Magnusson begins by understanding your aesthetic goals — whether that is increased volume, improved symmetry, or restoring fullness lost after pregnancy or weight change. He then assesses your existing breast tissue, skin quality, chest wall shape, and nipple position to determine which surgical approach is most appropriate. Implant type (silicone or saline), shape (round or anatomical), size, profile, and pocket placement (above or below the muscle) are all selected based on your specific anatomy and lifestyle. In Australia, AHPRA regulations also require a mandatory 7-day cooling-off period before any purely cosmetic breast surgery can proceed, giving you the time and space to feel fully confident in your decision.
What results can I realistically expect from breast augmentation?
Every patient starts from a different baseline — different tissue quality, breast shape, skin firmness, nipple position, and personal goal. Because of this, there is no single outcome that applies to everyone. A/Prof Magnusson takes a bespoke approach: the goal is always to create a result that is proportionate to your frame and consistent with what you set out to achieve, not a predetermined look. Outcomes are most predictable when your goals are clearly understood at consultation, when your anatomy is thoroughly assessed, and when implant selection is made collaboratively. Patients who have realistic expectations and a thorough understanding of the process consistently report higher satisfaction.
Will I need a breast lift as well as implants?
This is one of the most important questions to address before surgery, and the answer depends on your existing breast shape and nipple position. If your nipple sits at or below the lower breast fold, or if you have significant skin laxity, implants alone may not achieve the result you are looking for — a breast lift (mastopexy) may also be recommended. A lift repositions the nipple and tightens the surrounding skin, but involves additional incisions and scars compared to augmentation alone. A/Prof Magnusson assesses these factors at your consultation and will give you an honest recommendation about whether augmentation alone is appropriate, or whether combining it with a lift will produce a better outcome.
Can breast augmentation be combined with other procedures?
Yes, in appropriate candidates. Combining procedures is often called a “mummy makeover” when breast surgery is performed alongside body contouring. Common combinations include breast augmentation with abdominoplasty (tummy tuck), arm lift, or body lift. Combining procedures can reduce total recovery time and the number of general anaesthetics required. However, not everyone is suitable — factors such as age, weight, fitness, and medical history all influence whether it is safe to proceed with combined surgery. A/Prof Magnusson will discuss this openly during your consultation, with your safety as the primary consideration.
How is breast augmentation surgery performed, and what is the 14 Point Plan?
Breast augmentation is performed under general anaesthetic, typically as a day surgery procedure. An incision is made — most commonly in the fold beneath the breast (inframammary) — and the implant is placed either above the chest muscle (subglandular) or partially beneath it (dual plane), depending on your anatomy and goals. A/Prof Magnusson performs all breast implant surgery using the evidence-based 14 Point Plan, a set of antimicrobial protocols designed to minimise bacterial contamination of the implant at the time of surgery. Bacterial contamination has been linked to serious complications including infection, capsular contracture (scar tissue hardening around the implant), and — based on available evidence — may be associated with Breast Implant-Associated Anaplastic Large Cell Lymphoma (BIA-ALCL). All of A/Prof Magnusson’s breast implant patients are also registered on the Australian Breast Device Registry (ABDR).
Is breast augmentation surgery safe?
Breast implants are among the most extensively studied medical devices in history, in use since the 1960s and subject to ongoing regulatory scrutiny in Australia through the Therapeutic Goods Administration (TGA). When performed by a qualified Specialist Plastic Surgeon — a Fellow of the Royal Australasian College of Surgeons (FRACS) — in an accredited facility, breast augmentation is considered safe for appropriately selected patients. As with all surgery, risks exist and include infection, haematoma, changes in nipple sensation, capsular contracture, and implant rupture. Longer-term considerations include BIA-ALCL (a rare lymphoma associated with some textured implants) and the possibility of future revision surgery, as implants are not lifetime devices. A/Prof Magnusson is a member of the TGA’s Breast Implant Expert Working Group and has published research on BIA-ALCL and breast implant safety, ensuring his patients receive advice informed by the most current evidence.